News
Deliberate Practice with the Surgical Female Pelvic Trainer for gaining and maintaining competence in OB/GYN Laparoscopic Surgery
12 April 2022
Minimally invasive surgery, also known as Laparoscopic surgery, was first used on animals in the late 1800’s. A German surgeon, George Kelling, first applied the technology to humans, publishing his results in 1910(1).
While further changes were gradual, mostly due to slow progression of needed video technology, the real uprising started when Laparoscopic removal of the gall bladder was introduced at an American College of Surgeons (ACS) meeting in 1989.1
Since then, Laparoscopic surgery has been increasingly accepted in the general surgery, urology, vascular, and gynecology specialties, and is now recognized as the gold standard for surgery when possible. The benefits of minimally invasive surgery are said to include “less postoperative pain, fewer operative and post-operative major complications, faster recovery, less scarring, less stress on the immune system, smaller incision, and for some procedures reduced operating time and reduced costs.”2
Training for Laparoscopic surgery has become an essential part of postgraduate surgical specialties. “Competence in laparoscopy surgery necessitates acquisition of skills such as navigation and manipulation of endoscopic instruments with abdominal wall acting as the fulcrum, camera handling, depth perception, screen video-hand-eye coordination, and tissue holding with manipulations. Acquiring this set of skills requires a stepwise deliberate practice and is usually associated with a long learning curve which necessitates a structured training.” 3
“The trainee should practice on simulators until they attain a benchmark level of performance before they are allowed to practice surgery on actual patients. Simulations provide an effective means of acquiring the laparoscopy skills in a nonthreatening environment with trainee's freedom to practice skills repeatedly without any issues of patient safety. Moreover, teaching laparoscopy skills is often challenging during the actual operations because of concerns for patient safety, varying complexity of cases, and extra time consumption in anesthetized patients.”3
Just as Laparoscopic surgery has evolved, the knowledge around how to train is now progressing. A recent study outlines four core components for an effective skill simulation training session:
- Exposure: Briefing about the assignment ahead
- Sequence: Gradual increase in complexity of tasks
- Feedback: throughout and/or following the simulation session
- Repetition: Deliberate practice to reinforce and improve education, competences, and performance. 3
Developing training specific to minimally invasive surgery in Obstetrics and Gynecology is also evolving. A Delphi Study conducted in 2020 identified the following specific OB/GYN skills as priority technical procedures to be integrated into a simulation curriculum for OB/GYN residents in training:4
- Basic laparoscopy
- Laparoscopy with salpingostomy
- Laparoscopy with salpingectomy
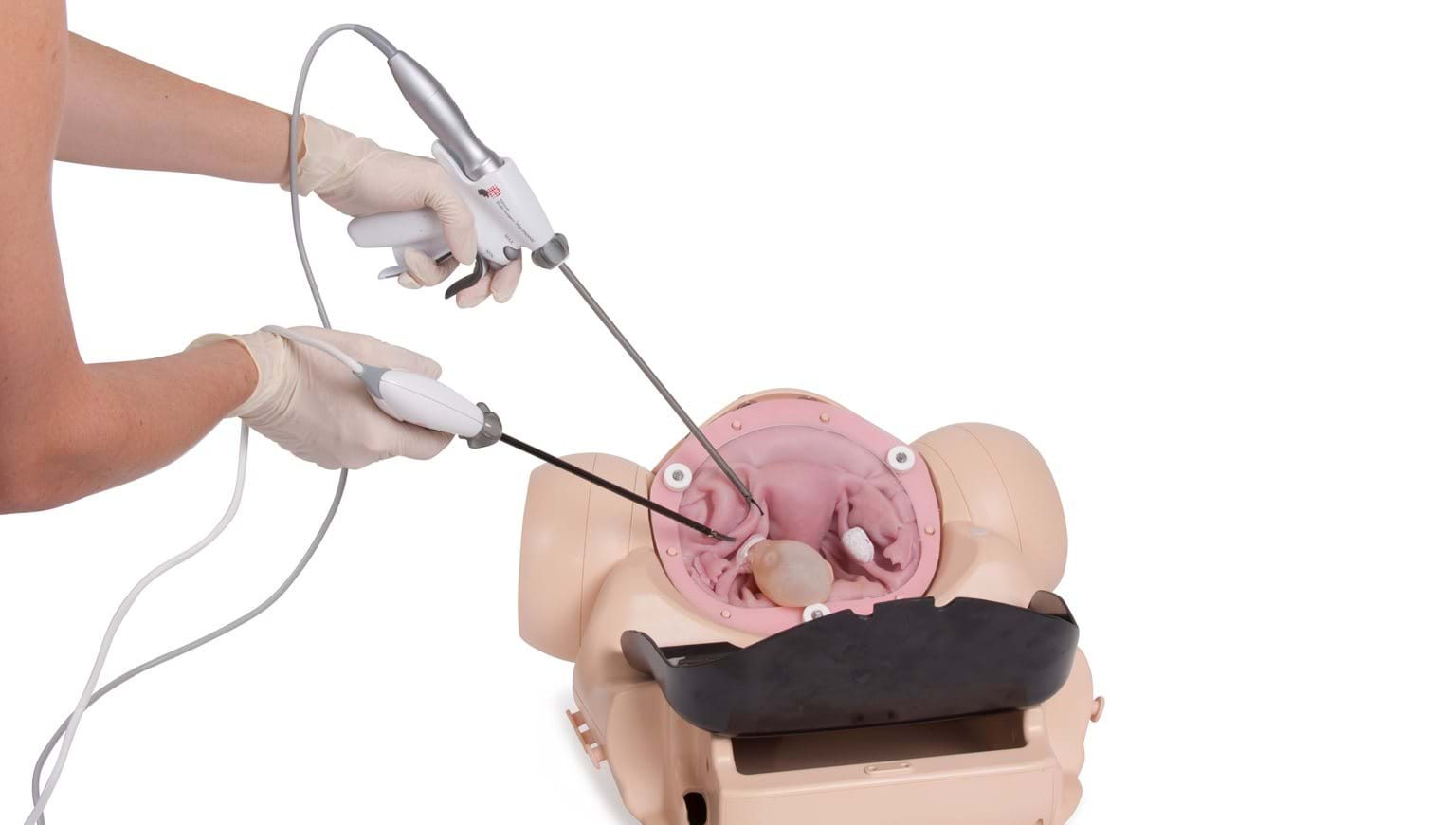
The Limbs & Things Surgical Female Pelvic Trainer (SFPT) is a comprehensive simulator that allows for training in the following fundamental skills as well as progressive increasingly difficult procedures needed for complete competency as an OB/GYN surgeon:
- Dissection down to and location of ureters
- Insertion and use of uterine manipulator
- Working with various gynecology instruments
- Identification of anatomical landmarks
- Salpingectomy: Removal of one or both fallopian tubes.
- Salpingostomy: Fallopian tubes are opened to remove contents, but the tube is not removed.
- Myomectomy: Removal of uterine fibroid non-cancerous tumors.
- Cystectomy: Removal of bladder
- Hysterectomy: Removal of uterus which may or may not include fallopian tubes and ovaries.
- Oophorectomy: Removal of one or both of the ovaries.
The SFPT, developed in collaboration with ACOG physicians, is also used in the ACOG Advanced Surgical Simulation and Endoscopic Surgical Simulation (ASSESS) course, which focuses on Laparoscopic hysterectomy, vaginal hysterectomy, and Midurethral [retropubic and transobturator] slings.
The need to be able to objectively assess performance to ascertain a surgeon’s competency has been increasingly cited in the literature. This objective assessment can be used to both test novice skills and to show maintenance of skills throughout a surgeon’s career. DeStephano et. al (2018), validated the use of the SFPT for global assessments of performance.5 Further work cited in 2020 showed that using simulation for skills training in OB/GYN Laparoscopic surgery “improved trainee performance measures in the operating room, decreases in the rates of avoidable complications, as well as improvements in feedback quality within the faculty-resident training dialogue”.6 Furthermore, the study showed that using a valid model, simulation can be combined with the Vaginal Surgical Skills Index to verify competence of both novice learners and practicing physicians.6
If you are interested in a demonstration of the Limbs & Things Surgical Female Pelvic Trainer, please contact us and our team will be more than happy to help.
USA
customerservices@limbsandthings.com
AUS
UK
1 The Evolution of Laparoscopy and the Revolution in Surgery in the decade of the 1990’s
2 Maximizing the benefit of minimally invasive surgery
4 A Nationwide Needs Assessment to Identify and Prioritize Technical Procedures in OB/GYN
5 Use of Limbs & Things Hysterectomy Model to Describe the Process of Establishing Validity
6 Chen CCG, Lockrow EG, DeStephano CC, et al. Establishing Validity for a Vaginal Hysterectomy Simulation Model for Surgical Skills Assessment. Obstet Gynecol. 2020;136(5):942-949. doi:10.1097/AOG.0000000000004085


