News
What Does it Take to be an Emergency Medicine Consultant Doctor in the UK?
09 November 2021
Led by the General Medical Council (GMC), the UK has a very transparent medical education infrastructure. The GMC has set standards and requirements for curricula that applies to every specialty. Their standards include excellence in the design and delivery of medical education and includes both technical and non-technical skills
Led by the General Medical Council (GMC), the UK has a very transparent medical education infrastructure. The GMC has set standards and requirements for curricula that applies to every specialty. Their standards include excellence in the design and delivery of medical education and includes both technical and non-technical skills. Students are first provisionally registered by meeting set outcomes for graduates and can become licensed once they meet requirements of core clinical and procedural skills.
Each royal college of medicine specialty has a curriculum committee that meets regularly and makes changes to their national curriculum. The GMC approves curricula and assessments for “65 specialties and 31 sub-specialties.”1 The GMC website lists core curricula and training pathways for undergraduate medical education as well as every specialty and subspecialty, easily viewable by anyone interested.
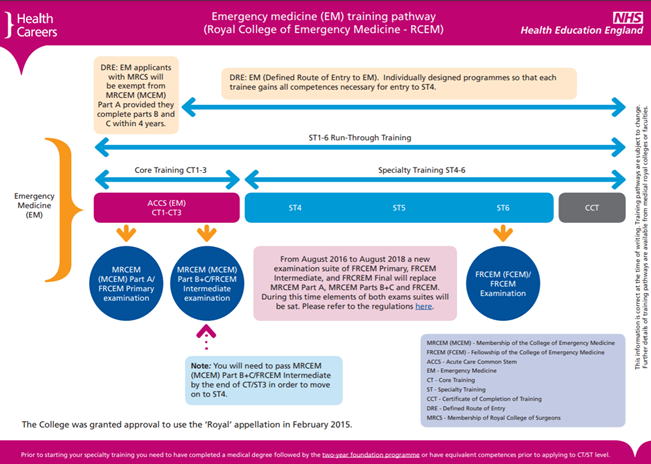
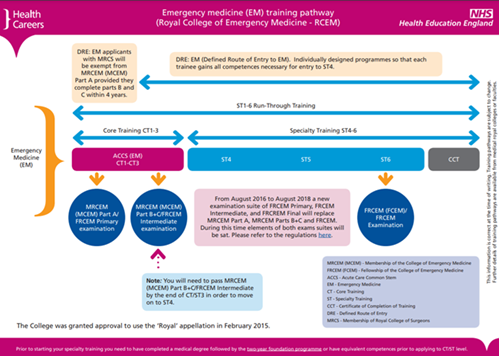
In August of 2021, the Royal College of Emergency Medicine implemented an updated curriculum for trainees. The scope of an Emergency Medicine Consultant is very broad, including rapid care of both adults and children needing physical or mental health care. The comprehensive curriculum expects the graduate to have “expertise in practical procedures related to the clinical care of… patients, will be expert communicators with strong interpersonal skills, strong emotional awareness and be adept at the management of potentially highly complex situations.”2 The curriculum contains 2 years of core training, 1 year of intermediate training, and 3 years of higher training to meet the Specialty Learning Outcomes (SLO) in 12 domains. The training pathway has been put into picture format by the NHS for an easy understanding of the training requirements:3
Simulation training, once seen as optional, is now required for Emergency Medicine training in the UK. Simulation can help to “ensure coverage of broader skills within EM” such as Point of Care Ultrasound (POCUS) techniques, normal delivery with a birthing simulator, opthalmology, Ear, Nose and Throat (ENT) examination, and fractures. According to the curriculum, “Procedural competency training, using simulation aimed at achieving technical competence for certain procedures should be provided as early as possible in in Acute Care Common Stem (ACCS) training and continue through all 3 stages of training. Scenario-based immersive simulation training is expected to be undertaken in in all relevant Specialty Learning Outcomes, with human factors incorporated into the scenarios where appropriate.”2
“Examples of simulation courses that should be used to deliver aspects of the curriculum include, but are not limited to:
ACCS
- Novice Anaesthesia Skills and Drills
- Assessment of failed intubation drill
- Vascular access
- Human factors
- Critical thinking
Intermediate and Higher Training
- Paediatric sedation
- Procedural skills- including emergency thoracotomy; emergency caesarean section, surgical airway
- Resuscitation team leadership
- Dealing with challenging situations in the workplace
- Human factors
- Critical thinking”2
Assessment of both technical and non-technical skills is also part of the updated curriculum. Using simulated patients and medium fidelity simulation equipment, all trainees will now be tested through a 16-station Objective Structured Clinical Examination (OSCE). This additional use of simulation allows faculty to be certain that the proper technical and communication skills are obtained for practice as an EM consultant.2
Limbs & Things is dedicated to providing anatomically correct, realistic models for procedural and team training. With over 20 products directly mentioned in the updated curriculum, we are certain that our range of products can help improve patient outcomes and the matriculation of successful, caring Emergency Consultants. For information get in touch with one of our team here.


