News
Developmental Dysplasia of the Hip (DDH) in the Infant
17 May 2022
"In some infants, the hip joint does not form correctly, causing what is now called DDH, or Developmental Dysplasia of the Hip, formerly known as congenital dislocation of the hip."
The human body has two sets of “ball and socket” joints. One is the shoulder, where the rounded head of the humerus (upper arm) bone fits firmly in a cuplike structure at the end of the scapula called the glenoid fossa. The other ball and socket joint is the hip, where the round head of the femur (thigh) bone fits tightly in the cuplike acetabulum in the pelvis.
In some infants, the hip joint does not form correctly, causing what is now called DDH, or Developmental Dysplasia of the Hip (formerly known as congenital dislocation of the hip or CDH1). In this condition, the acetabulum (hip socket) is shallow and does not allow for the femur to fit snugly in place, causing the newborn hip to be loose in the socket, or subluxatable, in mild cases, dislocatable in moderate cases, or in the most severe cases, dislocated.
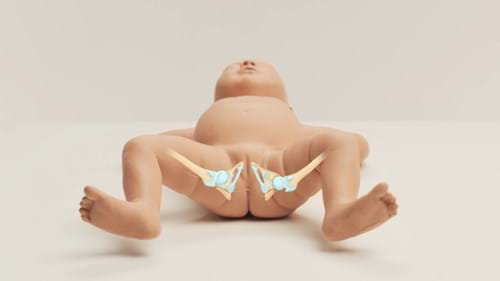
According to the International Hip Dysplasia Institute, 1 in 10 infants are born with hip instability, 1 in 100 infants are treated for hip dysplasia, and 1 in 500 infants are born with completely dislocated hips.5
Some risk factors of DDH include:
- Family history: 33% of babies with DDH have a blood relative who also had DDH.1
- Congenital disorders: Down Syndrome, Cerebral Palsy, or Spina Bifida increase the risk of DDH. 1,3
- Breech presentation: Frank breech (bottom presenting) increases the risk by about 20%, while complete or footling breech only increases normal risk by 2%.3
- Race: While there are few cases in Black, Chinese, or Korean children, white infants are most at risk.3
- Gender: Females are at greater risk than males.1,3
- Firstborn infants are more at risk than subsequent deliveries.1,3
Globally, infants are screened at birth and at most of their pediatric visits during childhood.3 This screening includes questions to the caregiver related to the risk factors as well as a physical examination of the hips. All newborn healthcare practitioners should be knowledgeable in performing the following tests:
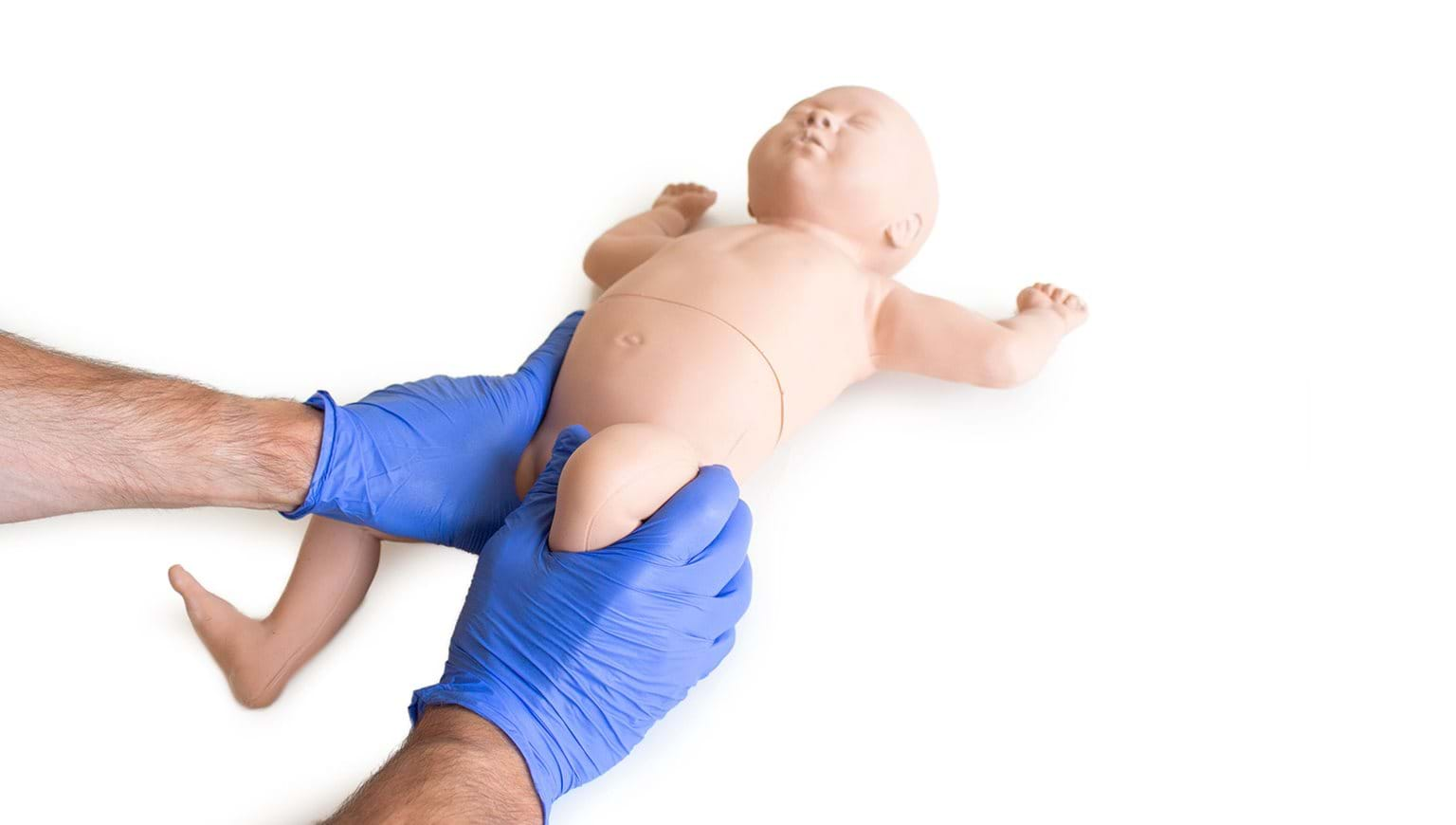
- “The Ortolani Test: The examiner’s hands are placed over the child’s knees with his/her thumbs on the medial thigh and the fingers placing a gentle upward stress on the lateral thigh and greater trochanter area. With slow abduction, a dislocated and reducible hip will reduce with a described palpable “clunk.”
- The Barlow Maneuver: This is done by guiding the hips into mild adduction and applying a slight forward pressure with the thumb. If the hip is unstable, the femoral head will slip over the posterior rim of the acetabulum, again producing a palpable sensation of subluxation or dislocation.
In infants, the degree of instability can be described as:
- Dislocated and reducible (+ Ortolani)
- Dislocated and irreducible (- Ortolani)
- Dislocatable (+ Barlow)
- Subluxed (a hip with mild instability or laxity with a – Barlow maneuver).”3
Once DDH is suspected, there is a growing trend of using Point-of-care Ultrasound (POCUS), in place of the traditional “formal sonography”4 to confirm the suspected diagnosis of DDH, prior to forming a treatment plan. During treatment, POCUS or formal Ultrasound may be used to “document reduction and follow the improvement or maturing of the dysplastic hip”.3 The American Academy of Pediatrics (AAP) “recommends and ultrasound study at six weeks of age for almost all baby girls who were in the breech, or bottom-first position.”5
Once the diagnosis is confirmed, patients are generally referred to a Pediatric Orthopedic Specialist for treatment. Treatment for more mild cases may be delayed for a few weeks, allowing the hips to become stable through normal growth and development. In more severe cases, early treatment is required.
With a goal of keeping the hips flexed and mildly abducted, a Pavlik Harness brace is generally prescribed, requiring frequent follow-up and adjustment as the infant grows. Normally, this harness is worn most hours of the day for at least 2-3 months, but the child is followed up much longer to be sure the treatment remains effective as they grow. If not diagnosed until 6 – 18 months of age, the child may be placed in traction, need surgery, or placed in a body cast for the required 3-6 month treatment time.
Limbs & Things is proud to announce the launch of our new infant hip exam model. While early diagnosis is key to ensuring that infants and their parents are made aware of abnormal findings, studies show that even Orthopedic surgeons or residents under their direct supervision misdiagnose up to 14% of dysplasia cases.6 Therefore, a model that teaches the correct method of performing the exam with realistic anatomy and haptic feedback will enable clinicians to correctly diagnose and treat infants at an early age.
If you are interested in knowing more please visit the product page. If you would like a demonstration of the new DDH model, please visit our request a demo page or contact customer services.
1 Better Health Channel Australia: DDH
2 Ortho Info: Developmental Dislocation (Dysplasia) of the Hip
3 Nationwide Children’s Department of Orthopaedics: Hip Dysplasia


