News
Using Medical Simulation to Improve Venous Access Skills
19 August 2022
In the USA alone, there are more than 300 million peripheral intravenous catheters (PIVC) sold each year “with at least 80% of all hospitalized patients receiving some form of infusion therapy.
In the USA alone, there are more than 300 million peripheral intravenous catheters (PIVC) sold each year “with at least 80% of all hospitalized patients receiving some form of infusion therapy. Even though it is a prevalent, technically difficult, and invasive procedure, most health care practitioners… receive little substantive peripheral vascular access education, training, or opportunities to practice skills until competent.
A recent analysis revealed overall PIVC catheter failure rates ranging from 35% to 50% leading to premature removal before the catheter's intended dwell time. Health care practitioner PIVC knowledge and skill deficits were identified as one of three primary factors leading to catheter failure and premature removal.”1
Skills training is a very important component of healthcare education. More and more, learners must complete competency based or mastery training prior to performing a procedure on a patient. These skill “check-offs” often happen in a simulation center using task trainers. Evidence now shows that not only does the training improve patient outcomes, but learners also gain confidence and enjoy the simulation experience.
In medical education, “the Accreditation Council for Graduate Medical Education (ACGME) has acknowledged and heavily emphasized the importance of clinical skills by establishing the patient care competency, which requires that gradate medical education trainees perform competently all medical and invasive procedures considered essential for their area of practice.”2
The support services of Phlebotomy and peripheral intravenous access placement skills are included in the ACGME requirements for all specialties.3 While physicians are trained to perform these skills, it is generally nurses who are tasked with the insertion, ongoing care, and removal of intravenous catheters.
“Peripheral intravenous catheter insertion remains a fundamental nursing skill that is largely learned during the post educational period in the clinical setting. Rigorous training and reinforcement mechanisms must be instituted in health care organizations to ensure continuous clinical proficiency with this skill.”1
Skill deficits that can be addressed in the simulation environment include “patient assessment, insertion site selection, catheter selection and insertion, catheter securement, dwell time, complication identification and treatment, and compliance with best practice guidelines.”1
A study conducted in 2011 “found that participants who received simulation based training had a significantly lower number of IV insertion attempts per patient compared with those who received traditional training. In addition, the number of reported patient complications was lower with the simulation based trained nurses (21% vs. 33%).”1
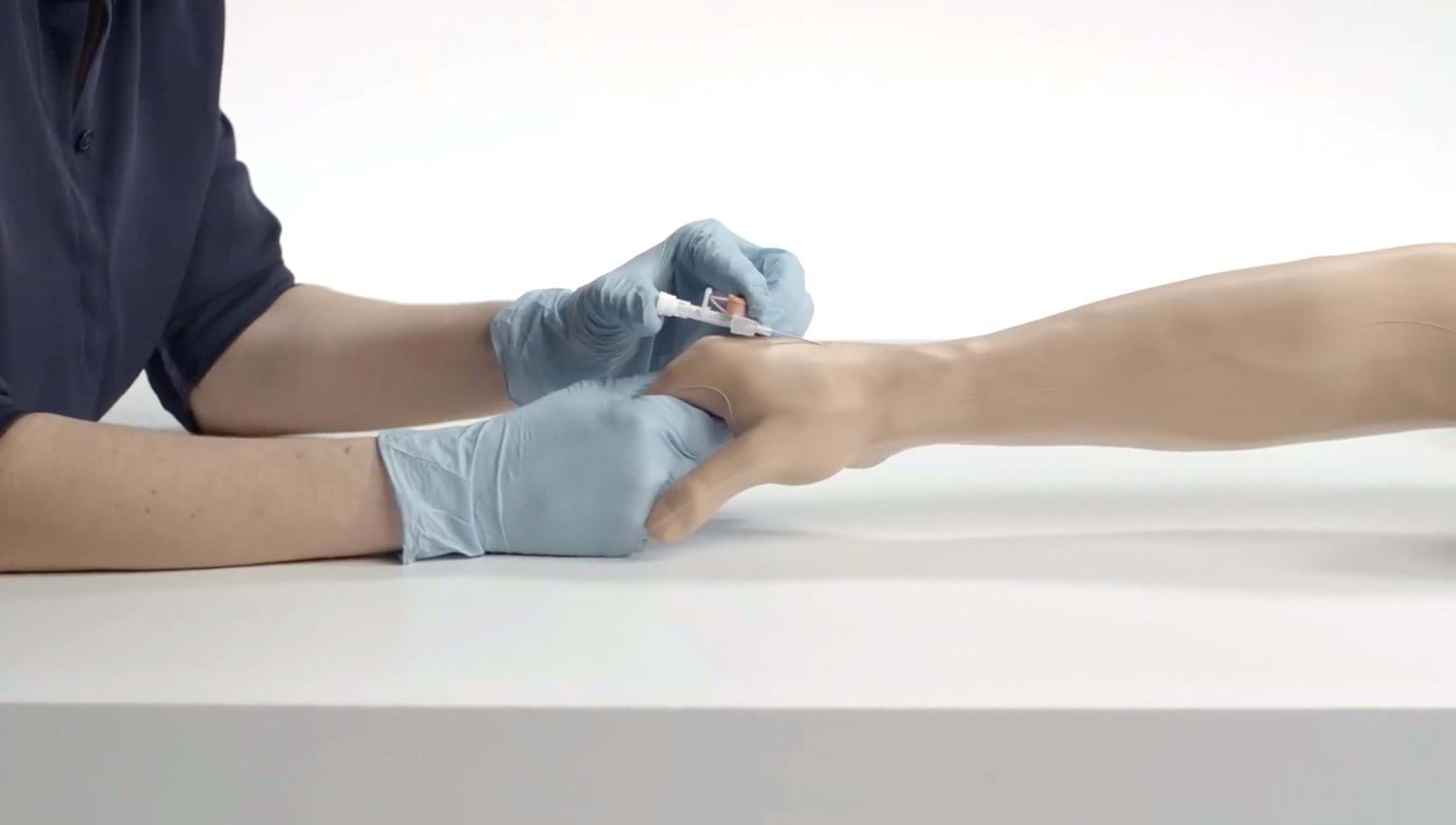
“The Advanced Venipuncture Arm (Limbs & Things LTD, Savannah, GA), a realistic adult task training arm with multiple access sites and controllable blood flow, was used”1 after a didactic session related to peripheral venous access. “Using this higher fidelity task trainer, participants performed and practiced all steps within the IV insertion process using all necessary IV supplies. Through guided practice, the process of PIVC insertion and use of supplies were brought together completely in simulated insertions. Participants completed six simulated PIVC insertion procedures on the Advanced Venipuncture Arm.”1
Interestingly, “Participants in this study showed significant increases in knowledge immediately after completion of the training program. However, knowledge scores significantly decreased upon follow up in the first group exposed to the intervention” at 2 months and 4 months after the course, “although scores remained higher than at baseline.”1 This finding reinforces the evidence that ongoing practice in a safe environment should be mandated for all healthcare practitioners called to perform venipuncture or peripheral intravenous access.
Limbs & Things has a variety of realistic, evidence-based training models that allow for every step of training needed to meet the standard of care for venipuncture and vascular access. The range of products includes both free standing and hybrid products which allows for enhancing communication skills as part of the procedure. If you are interested in knowing more, please visit the product page.


